Par's Story - Congenital Diaphragmatic Hernia (CDH)
The night before my 20 week ultrasound I was reading in my pregnancy book about what the doctor will be looking for and happen to learn of a birth defect I have never heard of – Congenital Diaphragmatic Hernia. The next day at the ultrasound we saw our baby for the first time and noticed the ultrasound technician seemed to do some extra looking and measuring. She said the baby’s stomach looked a little too close to the heart. Our baby had been moving around and looked just fine to us on the ultrasound--so even though we were first time parents, I wasn’t too concerned. My OB came in and said that after reviewing the ultrasound she is pretty sure our baby had something called CDH—then she and I said “Congenital Diaphragmatic Hernia” together. She was surprised I knew the name, and I explained that I only just learned about it the night before in my pregnancy book. I then attempted to reassure Rusty that it was going to be fine- they would just have to sew up the hole! My OB didn’t correct me—she just said that it is a serious matter and we would be referred to the high risk OB at the University of Alabama (UAB) at Birmingham. We were scheduled for the next day. Then we googled it and learned what it really meant—we were in shock. We hoped that our High Risk (HR) appointment would show that the ultrasound had been wrong and our baby was just fine. Our HR appointment told us we were having a baby boy and also confirmed CDH. They told us to think about our options, that a lot of people terminate with this diagnosis—because there is just such a small chance of survival.
Our only option was to find the best chance for our son. We found CHOP’s video advertisement on CDH babies, boasting an impressive survival rate, and we immediately made an appointment for a second opinion. At the time, they required an amniocentesis, so I reluctantly got one. In the meantime, we learned about Dr. Kays from my husband’s roommate from college—his brother had been a resident under Dr. Kays a few years earlier. He was emphatic that if we wanted our child to survive AND have any quality of life, we had to go to Dr. Kays. (Ironically, 5 years later, my husband’s friend would have his own CDH baby.) We reached out to Dr. Kays, and he responded with a telephone call. This call changed everything—this conversation was more than a well done video—it was hopeful but also honest and real. He told me that every decision he makes, he is thinking about our child’s brain. We made plans to meet with Dr. Kays and cancelled our CHOP plans. We made it to Dr. Kays at 26 weeks, a magic number for measuring the Lung to Head Ratio (LHR), among other things. Just 2 weeks prior, UAB had given us a LHR of .5 and a 5% chance at life. Dr. Kays gave us a LHR of 1.23 and 90% survival chance--but he made sure we understood that it really is just impossible to know—every baby is different. The discrepancy in theLHR was troubling. We returned home and continued meeting with UAB doctors making sure we knew all of our options here in Birmingham—but the continuity of care that Dr. Kays spoke of just seemed too important, and we knew UAB just couldn’t offer that—so we decided that I would deliver our baby at Shands Hosptial at UF with Dr. Kays. At 36 weeks, we left Birmingham, Alabama and relocated to Gainesville, Florida—and began waiting with LOTS of doctor appointments.
October 31, I had my 38th week check-up, and we scheduled my induction for November 7th. At midnight on November 1st, my water spontaneously ruptured—it was time. We headed to the hospital, I labored without pain medication while on Pitocin trying to start labor—by the 11th hour, the baby looked in distress, and they did an emergency c-section. Dr. Kays walked into the delivery room literally as they were lifting my son out of my belly—little did I know Dr. Kays got on a plane from Las Vegas when I had arrived at the hospital in labor. My son did not cry—but he was beautiful. Dr. Kays waved his little baby hand at me and said “See you later mom!” as he rushed him out of the delivery room to the NICU.
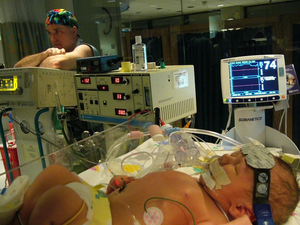
Par was immediately intubated and the honeymoon period began. He seemed so perfect on the outside. Our short term goal was to stay alive and stay off ECMO—Dr. Kays literally slept at his bedside for the first 2 days and then when he left, Par started going downhill. The ECMO machine was brought into his room but with a few tricks, we held off. Then one night Par got really sick—they called us in the middle of the night and told us he was going on ECMO—when we arrived at the hospital, they had blood circulating in the ECMO machine and had already done the procedure placing the cannulas in Par’s neck – but Dr. Kays said he had pulled out his final trick and by the grace of God, Par had stayed off ECMO—but during this time, his numbers went way down. Dr. Kays just didn’t know how it affected his brain—but for now we had avoided ECMO—if it happened again, we have no other options but ECMO. Two days later they removed the ECMO machine from his room. On day 8, he had his repair surgery where Dr. Kays removed the cannulas in his neck and put in a gore-text patch where his diaphragm was supposed to be. Par was missing almost all of his left diaphragm—his liver, kidneys, stomach, intestines—everything was up there. Dr. Kays cautioned that we had to watch the incision area closely because it could necrotize and because there really wasn’t enough skin to close his belly now that it was full of organs! Thankfully, it stayed closed and healed. The surgery was over and now we just had to wait for his lungs to start working properly. Slowly but surely, Par’s lungs began to improve each day!
Par was extubated at 28 days old and went on CPAP—this was the first time we ever held him. After about a week, he was changed to a nasal cannula then moved to the step down unit where we worked slowly and tirelessly on feeding and care. Finally, at 58 days old, 2 days after Christmas, we were discharged. Par left the NICU on a myriad of medication for reflux, fluid, and oxygen—but thanks to the wonderful occupational therapist/lactation consultant, he also was breastfeeding.
Par was walking at 9 months old, talking in complete sentences at a very early age, and reading before his peers. Par wasn’t on the growth chart until he was 5 and even now he keeps to the 5% range. He is excelling in school and LOVES all sports—especially contact sports! His endurance is better than most kids his own age- he is an incredible soccer player and as luck would have it, he is pretty good at golf, too! We thank God daily for this miracle who is constantly talking, driving us crazy about college sports scores, and wanting to play outside 24/7. We owe not just Par’s life, but his quality of life to the dedication of Dr. Kays. We often joke at our follow-up visits that Dr. Kays fixed him too much!
We currently live in Birmingham, Alabama.
For our entire documented journey: www.babyrich07.blogspot.com